Inflammation plays an intricate role in the development of health conditions, including in the development and progression of type 2 diabetes and prediabetes.
Inflammation is involved in type 2 diabetes as both a cause and a consequence, meaning that initially inflammation may trigger the development of diabetes, but also once you have diabetes, ongoing inflammation in the bodies cells contributes to various symptoms or complications.
Therefore, if you want better blood sugar and health results, focus on reducing inflammation in the body.
But what is inflammation exactly, you may ask? That’s a great question.
Let’s delve a little deeper and explore the answer.
What is Inflammation?
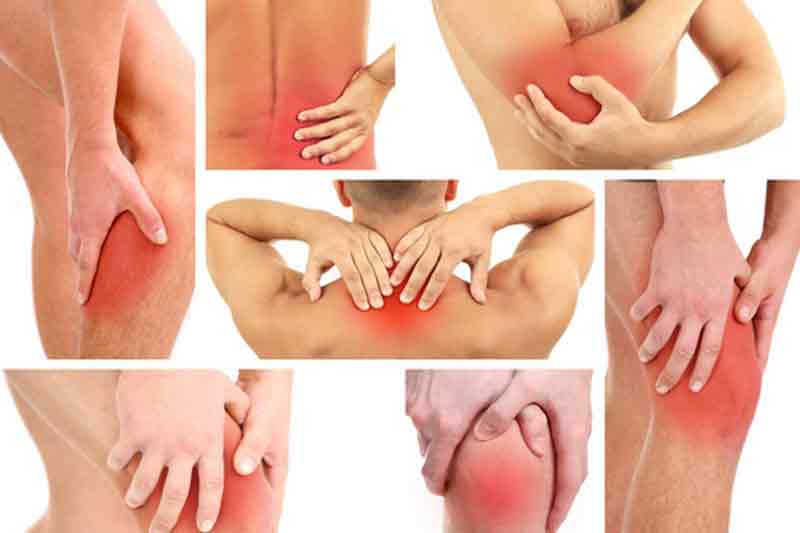
Inflammation is the bodies natural response to injury, stress, and trauma. It’s a natural response from our immune system that something isn’t right and the body needs some extra help to deal with the problem.
Think of a time you may have cut yourself. This is a sudden trauma where your immune system gets triggered, sends in all the helper cells to heal the wound, and once the job of healing is done everything goes back to normal. This is acute inflammation.
Chronic inflammation is delayed, persistent, and ongoing inflammation. This is something we can’t see because it occurs on a cellular level throughout the entire body.
With many of the modern lifestyle ‘stressors’ today it is not uncommon for us to develop a low grade inflammation throughout the entire body as the body tries to fight the many incoming stressors and traumas to body cells.
Increased Inflammation Precedes Type 2 Diabetes
Before type 2 diabetes develops there is increased production of inflammatory molecules in the bodies cells. While this seems bad, think of inflammation as a protection mechanism because that’s what it is – it’s your body trying to protect itself from too many changes occurring on a cellular/metabolic level.
Many health symptoms and the development of health conditions is the beacon that’s sounding the inflammatory signal.
It’s also a well known scientific fact that fat tissue is very metabolically active. It doesn’t just sit there doing nothing, it actively produces hormones and pro-inflammatory molecules, too. Since many people have obesity or weight gain alongside the development of diabetes, this relationship can be a major contributor.
Overall the consensus in the scientific literature is that if you have higher levels of inflammatory molecules, you have a higher risk of developing type 2 diabetes.
Inflammatory molecules act on different areas of the body
Various clusters of inflammatory molecules can act on different parts of the body and produce an effect. You know that whole cause and effect statement?
Well here are a couple of examples of that concept.
- Inflammatory molecules (cause) act on the liver and promote dyslipidemia (cholesterol imbalances) with increased VLDL and decreased HDL (effect).
- Inflammatory molecules (cause) also act on the muscles and liver, promoting insulin resistance (effect).
Inflammation is a response of the immune system
As noted earlier, inflammation is a natural response and reaction of the immune system. In every instance of increased inflammation, immune cells called macrophages are the first cells to respond to the body’s needs. Macrophage cells produce pro-inflammatory molecules and these molecules are basically just signals that tell the immune system and the body what to do.
Many things can provoke an immune response, including:
- stress
- lack of sleep
- environmental
- chemicals
- poor diet
- and higher than normal blood sugar levels
As you can imagine, if we keep on loading up one side of the scale, eventually somethings got to give. If inflammation doesn’t cease, and it won’t if we keep loading the scale, then the cells in the body start changing and we start seeing more symptoms arise.
These symptoms can present themselves in many different forms, from high blood pressure, high cholesterol, increased weight gain, aches and pains, heart disease, diabetes, and the list goes on and on.
Immune cells invade the pancreas when inflamed
Our macrophage immune cells are directly related to the development of type 2 diabetes in that they have been shown to invade pancreatic tissue.
When the macrophages invade the pancreas, they then produce more inflammatory molecules, and this could potentially help destroy the pancreatic beta cells. Without these your body can’t produce insulin efficiently, and this hormone is needed for blood sugar control.
Inflammation can increase the risk of complications
Once you have a diabetes diagnosis, essentially your body is in a state of low grade chronic inflammation.
As you may (or may not) know there is a much greater risk of vascular complications.
These pro-inflammatory molecules damage tissues in the vascular system, in fat tissue, in the muscles and liver, and as we already pointed out, in the pancreas.
High blood sugar itself promotes inflammation that can damage the blood vessels and lead to risk of vascular complications. This is why we always encourage you to achieve and maintain healthy blood sugar levels – it prevents complications!
Dysfunction contributes to increased inflammation
I don’t mean to scare you with all this because believe me you can turn it all around but it does help to get a better picture of what’s happening in your body right?
If you understand what is happening to your body it empowers you to make the right changes and that’s a very good thing. 🙂
Take a moment to imagine if your body was working properly… you wouldn’t have high blood sugar, high cholesterol, high blood pressure, difficulty losing weight, or any of the other symptoms you may have.
But when your body is not functioning properly all of these ‘symptoms’ collectively add to increasing inflammation by promoting ongoing involvement of the immune system and it’s reactions. It becomes a kind of repetitive cycle in itself, especially if the stimulus isn’t stopped.
Our approach to diet not only incorporates foods that help lower and maintain blood sugar levels, but foods that help reduce inflammation and improve metabolic health!
Different mechanisms proposed to contribute to stress and inflammation in diabetes
Glucotoxity
Rising levels of blood glucose are toxic to the body. Even small changes in glucose levels years before the onset of type 2 diabetes can be toxic to pancreatic beta cells.
Lipotoxicity
With insulin resistance, long chain free fatty acid levels are increased and can impair pancreatic secretion and increase insulin resistance.
Oxidative stress
High glucose levels causes cellular stress that produces free radicals (reactive oxygen species) in the body. Pancreatic beta cells are particularly vulnerable to oxidative stress and increased oxidative stress is also central to the development of insulin resistance.
Endoplasmic reticulum stress
The beta cells have a component called the endoplasmic reticulum. Insulin resistance promotes more insulin production and this increases the amount of proteins traveling through the endoplasmic reticulum, causing increased stress on those cells and subsequent reactions.
All of these stressors can be caused by over nutrition (overeating) or poor nutrition!
Eating too much is a major contributor!
Eating too much of the wrong things like sugar, refined carbohydrates, processed foods and junk food.
What that means is you can change it!
You CAN Turn It All Around!
Reducing inflammation is the key to prevention and management of diabetes.
What can you do?
- Choose the right type of carbohydrates
- Focus on eating the right types of foods
- Use our meal planning service – we’re helping people change their lives every single day!
Food really is our medicine and like Dr Mark Hyman says:
If we can eat our way into something, we can eat our way out of it

Anti-inflammatory Boosters for Diabetes
There are some well known foods and agents that help lower inflammation.
Here’s a few of them:
Hopefully this info has helped you get a better picture about the relationship between diabetes and inflammation. And more importantly, some of the ways you can reduce inflammation in your body.
Please share this info around to help others – thanks!
References
http://diabetes.diabetesjournals.org/content/52/3/812.longhttp://www.medicalnewstoday.com/articles/270817.phphttp://www.diabetesselfmanagement.com/Blog/David-Spero/put-out-the-fire-of-diabetes-inflammation/http://www.ncbi.nlm.nih.gov/pubmed/18673007http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3917922/http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3917922/http://www.nature.com/nri/journal/v11/n2/full/nri2925.htmlhttp://chriskresser.com/how-inflammation-makes-you-fat-and-diabetic-and-vice-versa

I am 3 x breast cancer survivor and a lymphatic Leukaemia
I have type 2 and it’s been 2 years now
Last year dropped 22lbs
Now I have gained 6 lbs and craving sugars badly
Can you help me
Thanks alot
Hi Karen, if you need assistance with meal ideas/recipes our meal plans may be helpful to you.
Thank you will check it out
Merry Christmas
Karen
Thanks, the food list looks very helpful.
Ok, so how do I find the “Anti-Inflammatory” Diet which I need ?
Find our food list here Patrick. The diet we suggest is anti-inflammatory.
Your free download doesn’t work. I’ve tried 4 different times now and nothing happens
That’s odd Genevieve, we’ve had no complaints from anyone else. I will get Mandy to email a copy over.
I have just been diagnosed with type 2. I’m probably only 10 pounda over weight. High cholesterol and diabetes are hereditary for me. I’m already on cholesterol meds. I need help with carbs / calories. How many grams per day of carbs. Or how many grams per meal per protein grams.
Hi Judy, you’d probably find our Free 2 Week Carb Course helpful.