Table of Contents[Hide][Show]
Improving insulin sensitivity is one of the most powerful things you can do to lower blood sugar, stabilize your energy, reduce your risk of complications, and support long-term metabolic health.
Whether you’re in the early stages of prediabetes or have been managing type 2 diabetes for years, restoring insulin sensitivity isn’t just possible, it’s one of the key steps toward reversing the underlying dysfunction in your body.
Discover science-backed strategies that help your body respond better to insulin and use glucose more effectively.
LISTEN TO THE PODCAST
Support the podcast by leaving a 5-star rating and review on Apple, Spotify or our Website – Thank You!

Insulin Explained
Some people do become fearful even hearing the word “insulin” because it brings up scary associations.
But, insulin is simply a hormone the human body naturally makes. And we need it to survive.
The hormone insulin is made by the pancreas and it’s job is to facilitate glucose uptake by moving the sugar from the bloodstream into the cells to be utilized for a variety of purposes, most significantly, energy.
If there isn’t enough insulin, or it isn’t working properly, sugar will build up in the bloodstream – or in other words, you’ll end up with high blood sugar.
With type 2 diabetes and prediabetes, insulin metabolism is altered.
What happens is the body either:
- Does not accurately recognize elevated glucose, OR
- Is not producing enough insulin – poor glucose control causes an INCREASED production of insulin (hyperinsulinemia), which eventually leads to the beta cells (cells that make insulin) burning out and dying, OR
- (Most commonly) Cells become resistant to insulin, otherwise known as insulin resistance.
Insulin Resistance
Insulin resistance is a key metabolic factor that causes prediabetes and type 2 diabetes – meaning, it is present long before a person is diagnosed.
While your body can still make some insulin (though it may be less in some people), the bigger issue is that the body is unable to utilize the insulin correctly.
The cells in your body are “resisting” the work the insulin is trying to do and becoming “desensitized” to it. The body’s cells tune out to insulin and stop listening to it.
Picture insulin there at the door of the cell with the key, ready to bring in the glucose.
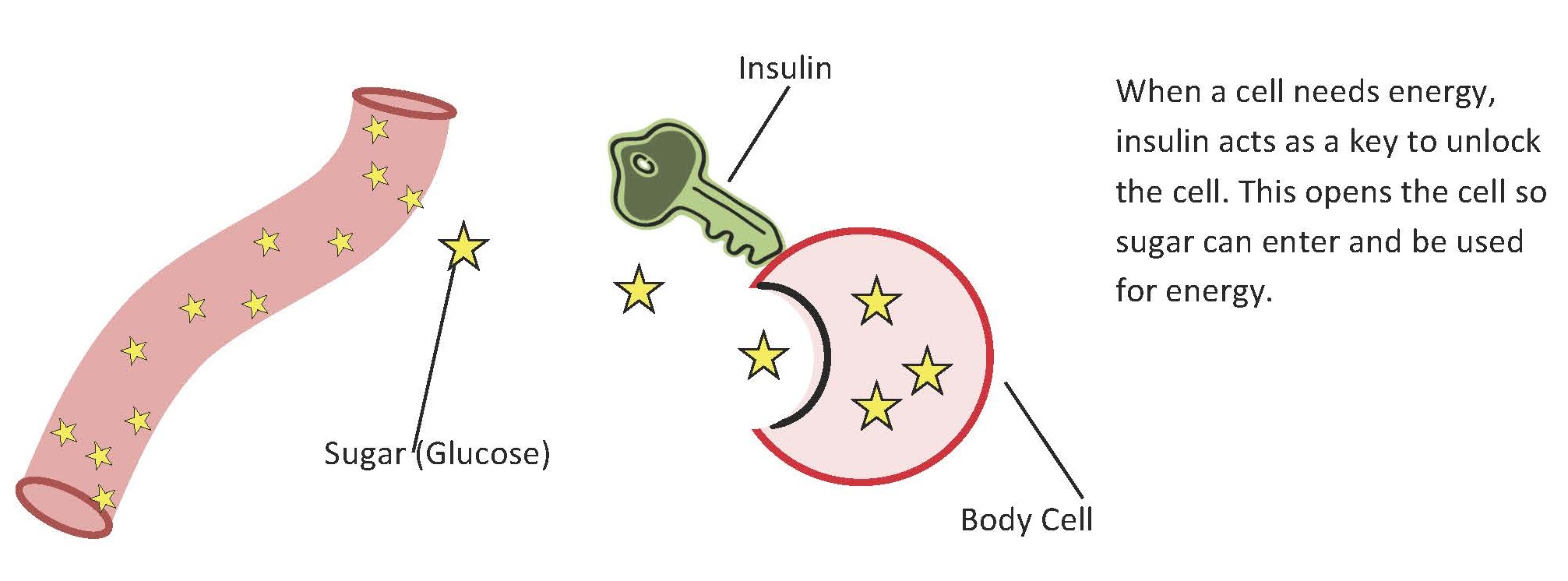
Under normal circumstances insulin unlocks the cell so that sugar/glucose can be moved out of the bloodstream and into the cells.
Now imagine the cell folding its arms saying, “nope, sorry, that key doesn’t fit anymore. I changed the locks.” That’s insulin resistance.
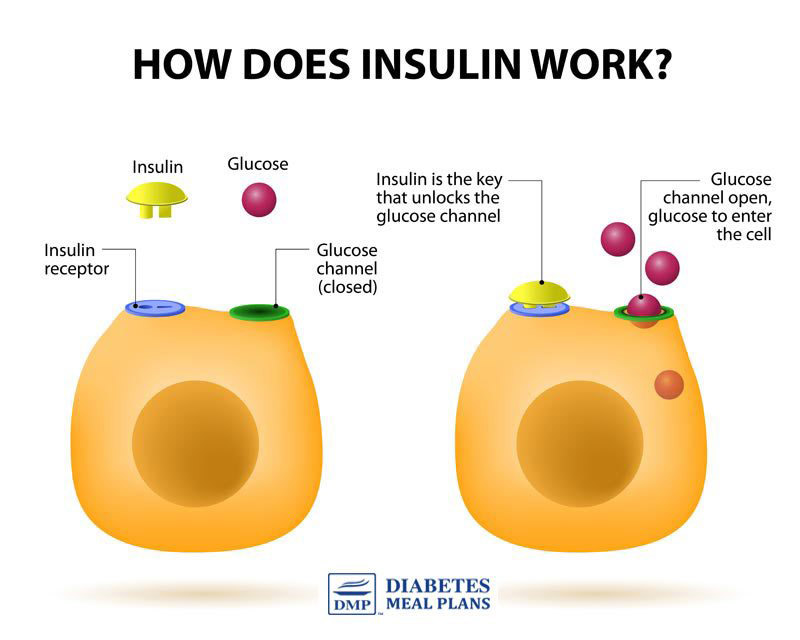
Rather than letting the glucose in, the cells no longer listen to the hormonal signals that are sent. So the more sugar that stays in the bloodstream, the more cells remain starved for energy.
As a result, the body tries to compensate by making more insulin – pumping more of it out from the pancreas to try to get those cells to unlock. But in many cases this doesn’t help. You simply end up with high glucose and high amounts of insulin circulating in the blood, which is toxic to the body.
Unfortunately, high insulin levels are linked with:
- Blood vessel damage
- High blood pressure
- Heart disease
- Cancer
In addition, weight gain is likely because when the insulin does work, it stores whatever it can get hold of, as body fat.
So overall insulin resistance contributes to:
- Diabetes
- Obesity
- Heart disease
- Fatty liver
- And many other chronic conditions
If a person is insulin resistant, it will essentially evolve into type 2 diabetes if lifestyle changes aren’t made, and sometimes even when they are.
Insulin resistance is the result of metabolic syndrome and can result from a combination of both lifestyle and genetic factors.
Risk factors include:
- Obesity
- Sedentary lifestyle
- Poor diet
- Steroid use
- Illness/infection
- Stress
- Poor sleep
- Smoking
- Genetic factors
- Age
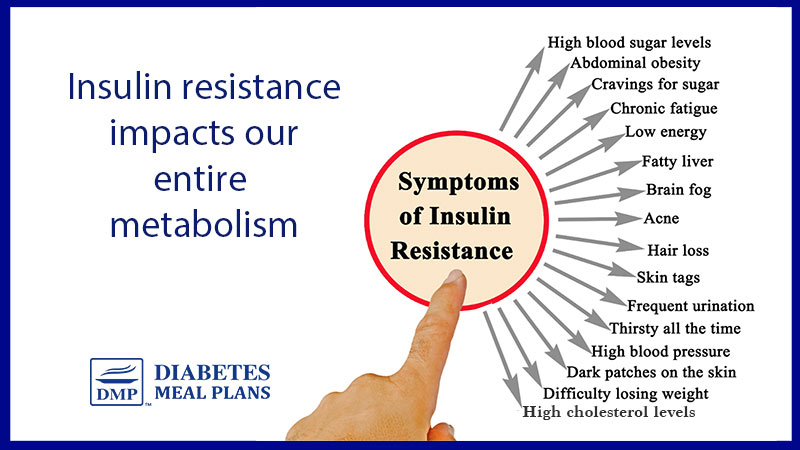
Insulin Sensitivity
Insulin sensitivity is the opposite of insulin resistance. It means that the body’s cells are very perceptive and responsive to the insulin signals produced.
While we don’t want to be overly sensitive to insulin, which can cause hypoglycemia very easily, for most of us, that isn’t a problem.
Really, for a person with type 2 diabetes or prediabetes, improving insulin sensitivity is your goal because it reduces your insulin resistance and improves the efficiency of the cells to take glucose – it helps that insulin key unlock those doors.
Insulin sensitivity can be measured by a blood test to detect circulating insulin, although doctors rarely order this test because treatment for high blood sugars is really the same anyway.

Ways to Improve Insulin Sensitivity
Improving insulin sensitivity doesn’t come down to one magic food, supplement or action. It’s a combination of consistent, proactive strategies that work together to support better metabolic health.
Based on the latest science, here are the core areas to focus on:
1. Cut Back on Processed and Refined Foods
- Remove added sugars, refined grains, and packaged foods from your diet.
- These foods drive inflammation, increase insulin resistance, and place extra stress on your metabolic system.
- Also avoid inflammatory seed oils (soybean, corn, canola, cottonseed, etc.) and food additives and preservatives, which can disrupt gut bacteria and worsen insulin function.
2. Prioritize Natural Whole Foods
- Load your plate with non-starchy vegetables — the best source of carbs for people with insulin resistance.
- Include a wide variety of colors and types for optimal nutrients and fiber.
- Use fresh or dried herbs and spices, which contain natural compounds that support insulin action.
3. Eat Quality Protein at Every Meal
- Get adequate daily protein intake (around 25–30% of daily calories).
- Include lean meats, eggs, fish, dairy, tofu, tempeh, nuts and seeds.
- Protein helps preserve muscle mass, reduce inflammation, and improve metabolic function.

4. Focus on Healthy Fats
- Include more monounsaturated fats (like olive oil, avocado, macadamias, almonds).
- Add more omega-3 fats (from fatty fish like salmon, sardines, tuna, and seeds like chia, hemp, and flax).
- These fats reduce inflammation and improve insulin sensitivity in muscle and fat cells.
5. Support with Evidence-Backed Supplements
- Magnesium: Helps regulate glucose uptake and insulin signaling; often deficient in people with prediabetes and T2D.
- Berberine: Clinically comparable to some diabetes medications for improving insulin sensitivity and glucose regulation.
- Vitamin D: Important for insulin secretion and insulin sensitivity — test and supplement if deficient.
6. Move Your Body Regularly
- Physical activity increases muscle glucose uptake, restoring and maintaining insulin sensitivity.
- Combine aerobic exercise (like walking) with resistance training (like squats or leg lifts) for the best results.
- Aim for at least 30 minutes of movement most days of the week.
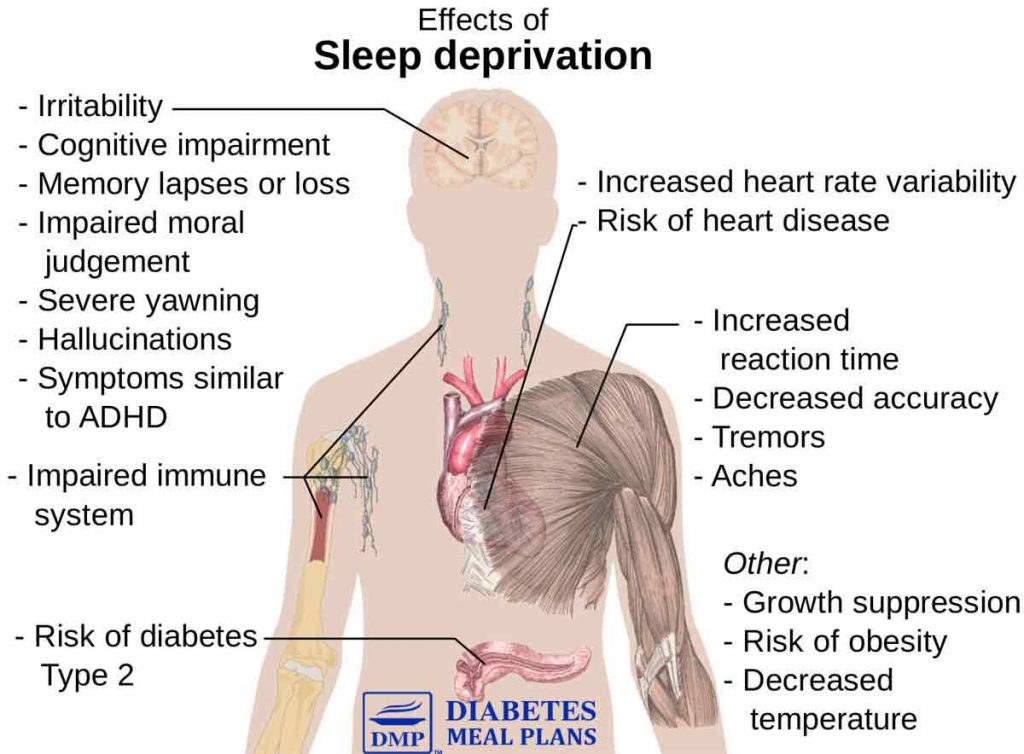
7. Prioritize Sleep
- Poor quality or short sleep increases insulin resistance, inflammation,] and cortisol.
- Aim for 7–9 hours of restful sleep nightly.
- Create a calm sleep environment and reduce screen time before bed.
8. Manage Stress
- Chronic stress raises cortisol and glucose levels, increasing insulin resistance.
- Incorporate stress-reducing practices like meditation, deep breathing, nature walks or gentle yoga.
- Even 10–15 minutes a day of mindful relaxation can help regulate your nervous system and improve insulin function.
9. Track Your Progress
- Monitor changes with simple lab tests: fasting insulin, fasting glucose, HbA1c.
- Watch for signs of improvement like reduced belly fat, more stable energy, improved sleep, and better blood sugar readings.
- Use a glucometer or CGM to see how your meals and habits affect your blood sugar over time.
When you combine these strategies, you build a strong foundation for improving insulin sensitivity, and it’s that steady, structured approach that leads to lasting results.



Barbara Funderburg
Just checking in. Great article.
Rhonda
Thanks for the info, FS 158 this morning – not good
Virginia
Checking in.
Great article
Malorie: Dietitian (MS, RD, CLT)
Thanks for checking in Virginia!
Ginger
Day 15 and my Fbs a.m. remained the same as yesterday …
I so appreciated the in depth article of information in understanding of improving insulin sensitivity/ resistance, this help immensely as well as the uses of the supplements…
Blessings
Ginger
Malorie: Dietitian (MS, RD, CLT)
Glad the information has been helpful to you! Thanks for checking in.
Robert Cooper
Best explanation I have ever seen and fully understandable. Well done. Many thanks.
laurie wilson
can you use metformin and berberine together
Jedha: Nutritionist (MNutr)
Yes you can but should consult your doctor about any supplementation. Research studies have shown that combined therapy can improve fasting glucose and A1c. Thanks for checking in Laurie.
Marlene
at bedtime last night BS 7.4 and this morning it was 8.4.
I am trying to eat more veg. I cooked cauliflower in the steamer yesterday and it was delicious. Nice and crunchy. This morning for breakfast I had leftovers from supper – steak, green beans and cauliflower. No food cravings all morning!
Jedha: Nutritionist (MNutr)
Good to hear Marlene – keep up that commitment. ;)
lynda
I have really learned a lot about diabetes just from your site. my mother had diabetes ,she pased in the 70’s and i have always felt guilty cause i did’t know much about this disease.even today it amazes me that people are not informed.thank you .I have tried some of the recipes and thanks again .I was so frustrated about what to make for meals.keep doing what your doing.
Jedha: Nutritionist (MNutr)
Thanks for your kind words Lynda. Glad everything is helping. :)
Kelly Wilson
Never really understood insulin sensitivity so this was so helpful. Thank you. Numbers are still doing well so now I’m hoping to continue working towards better health. Thank you so much! Great info!!
Jedha: Nutritionist (MNutr)
Glad you’re enjoying it Kelly. Thanks for checking in.
Tina Falconer
129 before bed, but 190 FBS this morning – why?
Jedha: Nutritionist (MNutr)
Did you check out the info on fasting blood sugar Tina – will explain why this may happen.
Gerry
Great article. Thank you! Need to read several times so this concept really ‘sinks’ in. You explain it very well and simply.
Emily - Dietitian (MS, RD)
Thanks for the positive feedback!
Margaret
Very informative article. I have spent this am reading articles in the library section. I have found answers to many questions that I have had for years.
Ellen
Checking in.
Kept to my plan. going good
Malorie: Dietitian (MS, RD, CLT)
Glad everything is going well-thanks for checking in!
Carol
FBS 135 Thank you for your comments about snacks and carbs. Today’s article about improving insulin sensitivity was helpful.
Bill
This is a great article and broken down for me to grasp. It reminds me of signs in my past (fatty liver deposits) 20 years prior to being termed a T2 diabetic. With those findings I did not receive any help from medical professionals until I had a very old type 2 PA that told me try 4 oz servings of fish, turkey, or chicken accompanied by green leafy veggies, only. Once I took his advice my AST dropped from 124 to 75 and my ALT dropped from 132 to 41 (within range)
Jodi
Great article about resistance.
FBS today 151
MARY
I am 74 year female and was diagnosed with type 2. I have not been able to locate a dietitian in my area. A RN at Dr office with some knowledge gave me a sample menufor one day. This came from the ADA, it suggested I eat 30 grams of carbs per meal and snack. This is way too much for me. Could you help me please?
Jedha: Nutritionist (MNutr)
Hey Mary, 30 grams per meal is pretty high, ADA guidelines have always been steep – at least they’ve come down from the 45 grams they were recommending just a year ago! This info here might be useful.
Susan Lim
Thank you so much for sharing such an enlightening article!
Lori
Great article! Thanks for the inspiration!
Abeer
Thank you so much, I really appreciate sharing such an informative article.